
ACA Plans Without Provider Networks: What Consumers Need to Know
This article was written by Kate Spilsbury, licensed health insurance broker and owner of Mere Benefits, who helps individuals and families navigate Medicare, Marketplace, and private health insurance options.
A recent healthcare policy proposal has sparked a lot of discussion among insurers, brokers, and policy experts.
The idea being discussed is the possibility of allowing Affordable Care Act (ACA) Marketplace plans without traditional provider networks.
At first glance, that might sound like innovation or increased flexibility in healthcare coverage.
But the reality is more complicated.
Understanding how these types of plans might work—and how they could affect premiums, subsidies, and access to care—is important for anyone who relies on Marketplace coverage.
As someone who works with consumers navigating health insurance every day, I see how complicated these systems can be behind the scenes.
Let’s break down what this proposal could mean in practical terms.
How Traditional ACA Health Plans Work
Most ACA Marketplace plans today operate using provider networks.
A provider network is a group of doctors, hospitals, and healthcare facilities that have negotiated contracts with an insurance company.
These contracts establish:
negotiated prices for services
billing rules
reimbursement rates
cost-sharing structures for patients
For consumers, the experience typically looks like this:
Find a doctor in the plan’s network
Show your insurance card
Pay your copay or deductible
The provider bills the insurance company directly, and the negotiated rates apply automatically.
This system provides a level of predictability for consumers, even though it can create administrative complexity behind the scenes.
What Are “Non-Network” Health Plans?
The proposal currently being discussed would allow ACA plans that do not rely on traditional provider networks.
Instead of negotiating contracts with doctors and hospitals, the insurer would publish a fixed payment amount for certain services.
For example:
Office visit → $100
MRI → $800
Surgery → $5,000
A patient could then visit any provider willing to accept that payment amount.
If the provider charges more than the amount the plan pays, the patient would be responsible for the difference.
This model shifts some of the pricing negotiation from the insurer to the patient.
Supporters argue that this could increase competition and encourage providers to offer more transparent pricing.
Critics point out that it could also expose consumers to additional financial risk.
Similar Models Already Exist: Indemnity Plans
It’s important to understand that this concept is not entirely new.
Versions of this model already exist today through what are known as indemnity health plans.
Indemnity plans typically pay a fixed dollar amount for covered services, rather than negotiating provider networks.
For example:
A plan may pay $100 for an office visit
$800 for an MRI
$1,000 per day for a hospital stay
The patient pays the provider directly and then receives reimbursement from the insurance company according to the plan’s payment schedule.
If the provider charges more than the amount covered by the plan, the patient pays the difference.
While these plans can work for some individuals, they were never designed to function as ACA-compliant coverage.
They often require patients to:
negotiate healthcare pricing themselves
pay providers upfront
manage reimbursement claims
That level of involvement can be difficult for many consumers.
Challenges in Rural Areas
One of the biggest concerns with a non-network model involves provider availability, particularly in rural areas.
In areas with limited provider options, patients may have little negotiating leverage.
If only one hospital or provider group serves the region, patients may have no choice but to accept the provider’s pricing.
Without negotiated networks, there is no guarantee that providers will accept the payment amount offered by the plan.
This could make access to care more complicated in communities that already face healthcare shortages.
Reference-Based Pricing Explained
The concept being discussed in policy circles is often referred to as reference-based pricing.
In a reference-based pricing system, the insurance plan sets a benchmark price for healthcare services.
The plan may base those prices on a percentage of Medicare reimbursement rates or another pricing standard.
Patients then seek care from providers willing to accept those rates.
In theory, this could encourage healthcare providers to compete on price.
In practice, however, it requires consumers to understand pricing structures and sometimes negotiate with providers directly.
That level of engagement is unfamiliar to most people navigating health insurance today.
The ACA Subsidy Benchmark Issue
One of the most overlooked aspects of this proposal involves how ACA subsidies are calculated.
Marketplace subsidies are based on the cost of the second-lowest-priced Silver plan in a region.
This plan is known as the benchmark plan.
The lower the benchmark price, the lower the subsidy amount consumers receive.
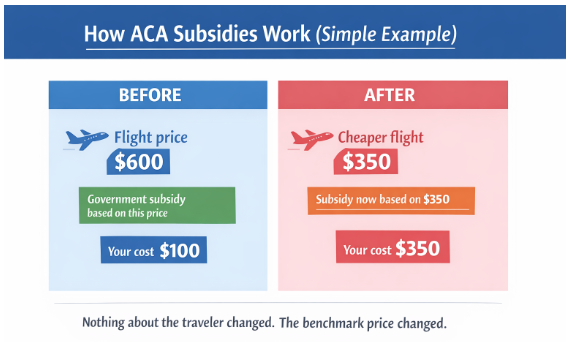
Here’s a simple way to think about it.
Imagine airline tickets.
If most flights cost $600, subsidies are calculated based on that price.
But if a new airline enters the market offering a basic ticket for $350, the benchmark price drops.
Even if you still want the $600 ticket, your subsidy may now be based on the $350 option.
The same concept applies to ACA plans.
If very low-premium plans enter the market and become the benchmark, subsidy amounts could decline.
That could make traditional plans with provider networks appear much more expensive after subsidies are applied.
Network Challenges Already Exist Today
It’s also important to acknowledge that provider network challenges are already one of the most common frustrations consumers experience with ACA coverage.
Even when someone checks a provider directory before enrolling, things can still change.
Doctors move practices.
Provider groups renegotiate contracts.
Offices stop accepting certain plans.
Sometimes provider directories themselves are inaccurate.
These changes can happen mid-year, leaving patients scrambling to find new providers.
While removing networks entirely may not solve these issues, it does highlight how complicated the current system has become.
The Bigger Issue: Healthcare Pricing Transparency
At the heart of this conversation is a larger problem.
Healthcare pricing in the United States is often highly opaque.
The same medical procedure can cost dramatically different amounts depending on the hospital, insurer, or negotiated contract involved.
For example, an MRI may cost:
$900 at one hospital
$4,500 at another
Without transparent pricing, it is extremely difficult for consumers to shop for care effectively.
Until healthcare pricing becomes more transparent and predictable, many policy proposals may simply shift complexity from one part of the system to another.

When These Models Might Work
Non-network or reference-based pricing models may work best for individuals who:
prioritize lower premiums
are comfortable asking providers about pricing
rarely use healthcare services
understand potential balance billing risks
For some consumers, these trade-offs may be acceptable.
When They May Not Be the Best Fit
These types of plans may be more challenging for individuals who:
have chronic health conditions
require frequent medical care
live in rural areas with limited provider options
want predictable copays and provider access
Understanding how a plan works before enrolling is extremely important.
Final Thoughts
Healthcare coverage decisions can have a significant impact on both finances and access to care.
Policy proposals like this often involve complex interactions between plan design, provider networks, and government subsidy calculations.
For most consumers, the goal is simple.
They want to know:
what their insurance covers
which doctors they can see
what their healthcare will cost
Understanding the details behind different plan structures can make it easier to choose coverage that fits your needs.
If you ever want help reviewing your health insurance options or understanding how Marketplace coverage works, our team at Mere Benefits is always happy to help guide you through the process.
Frequently Asked Questions
Are ACA plans without provider networks currently available?
Most ACA Marketplace plans today still rely on provider networks. However, policy discussions have explored the possibility of allowing plans that use alternative pricing models instead of traditional networks.
What is reference-based pricing in health insurance?
Reference-based pricing is a model where an insurance plan sets a fixed payment amount for medical services. Patients can visit providers willing to accept that amount, but may need to pay the difference if a provider charges more.
What is an indemnity health insurance plan?
Indemnity plans pay a fixed dollar amount for certain healthcare services rather than negotiating provider networks. Patients may pay providers directly and then receive reimbursement from the insurance company.
Why do ACA subsidies change from year to year?
ACA subsidies are based on the cost of the second-lowest priced Silver plan in each area. If lower-priced plans enter the market, the benchmark price can change, which affects subsidy amounts.

